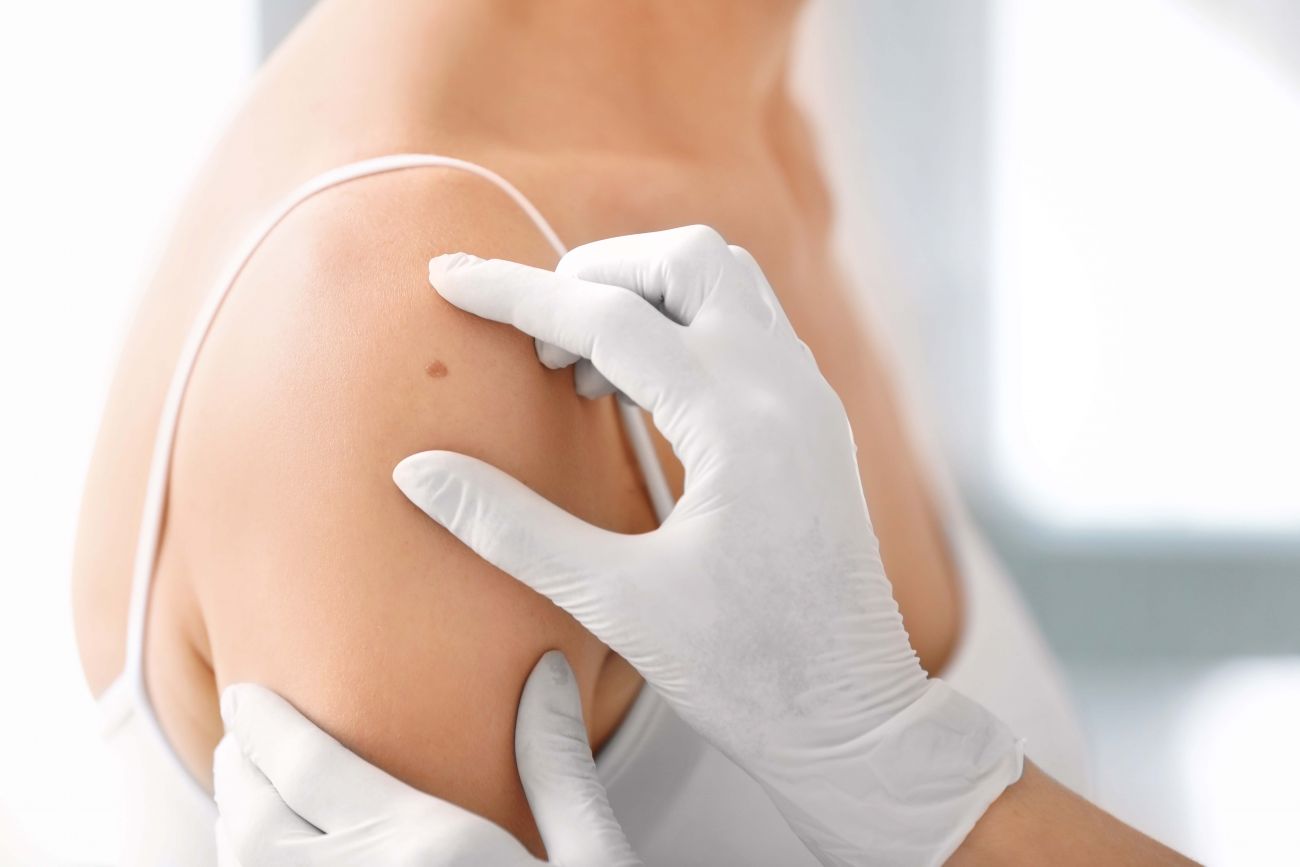
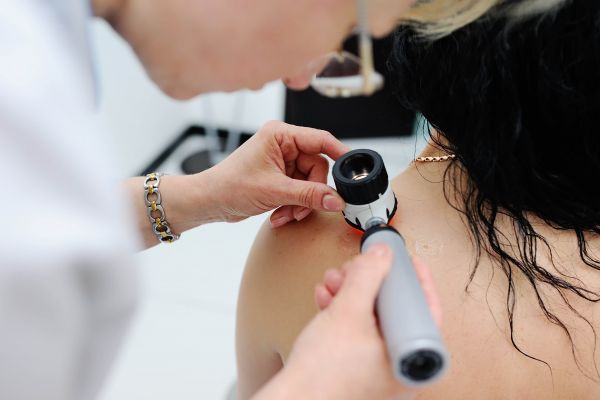
While it might be tempting to use the two words interchangeably, there are distinctions to be made between melanoma and skin cancer.
Melanoma is a type of skin cancer, but not all skin cancers are melanomas, explains Gyorgy Paragh, MD, PhD, Chair of the Department of Dermatology at Roswell Park Comprehensive Cancer Center. “To understand skin cancer, you have to look at different kinds of skin cancers. The best way to categorize them is what cell type gives rise to cancer; what cell type goes bad and forms the cancer. Most skin cancers are what we call keratinocyte carcinomas,” arising from the most abundant cells found in our upper layers of skin. Keratinocyte carcinomas are also often referred to as non-melanoma skin cancers, although the latter term also encompasses many rare skin cancers.
Within keratinocyte carcinomas, the two most common diagnoses are basal cell carcinomas and squamous cell carcinomas, and each of these has distinguishing characteristics as well. Basal cell carcinoma (BCC), the most common skin cancer, is a slow-growing cancer. BCCs emerge over time, usually as a pink, pearly spot or bump that bleeds easily, or as a small nonhealing ulcer. Surgery is usually curative for BCC; however, if BCCs are untreated, they may grow very large and destroy normal tissues. In sporadic cases, BCC may even spread to lymph nodes or other parts of the body. Squamous cell carcinoma (SCC) is the second-most common kind of skin cancer that arises from the keratinocytes (squamous cells), the most abundant cell in the skin. They often look like warty bumps or scaly patches on the skin and sometimes can also show up as an unhealing ulcer. SCC can sometimes spread to the lymph nodes and distant parts of the body.
Melanomas come in different types
Melanomas are cancers that arise from melanocytes and pigment cells that provide pigmentation to the skin. These cancers are rarer than keratinocyte carcinomas but are more likely to spread. Because of their propensity to spread, melanomas can more often become life-threatening. While officially designated as one class of skin cancer, Dr. Paragh says that “there are different subcategories of melanomas based on some clinical features that make the tumors different. Nevertheless, given their usually pigmented nature and similar determinants of risk, they are often categorized as one entity.”
Some melanomas — such as nodular melanoma and lentigo maligna melanoma — are most commonly found in the body areas where the skin has suffered chronic damage from exposure to the sun, such as the ears, face and neck. However, the most frequent melanoma type — superficial spreading melanoma — often starts in areas where the skin is intermittently exposed to the sun, and may have been badly burned a few times, like the middle of the back, the calf of the leg and on the chest.
“The areas where, during your childhood, maybe you had a couple of bad burns are usually going to be the sites for superficial spreading,” Dr. Paragh says. While nodular and lentigo maligna melanomas appear in similar sun-damaged areas, their growth patterns are distinct. “Nodular melanoma starts as a tumor that grows vertically very fast and therefore early on will be close to blood vessels and lymphatic vessels and thus is more likely to metastasize. Whereas lentigo maligna often spreads for a long time superficially and converts into the vertical growth pattern later to create a lentigo maligna melanoma, so you may have more time to catch it early.”
Cancer can also develop on seldom-exposed parts of the skin
It’s possible to develop melanoma in areas of the skin that rarely get exposed to the sun. Acral lentiginous melanoma occurs on the soles of the feet or palms of the hand, around or under the nails. “Acral lentiginous melanoma is not driven by prior sun damage, and these melanomas are common in people with different skin types. Sunburns are thought to drive superficial spreading melanoma growth, so fair-skinned individuals are at a much higher risk of getting those than darker skin-type individuals. Still, as acral lentiginous melanoma comes uniformly to everyone, this is the predominant type we see in darker skin-type individuals,” Dr. Paragh says.
Unfortunately, acral lentiginous melanoma occurs in unusual locations, where people do not expect to see skin cancer and do not often look for problem spots. Especially in people with darker pigmented skin, who are otherwise less likely to develop skin cancer, acral lentiginous melanoma can be harder to find at an earlier stage, when they’re easier to treat and less likely to spread. “While lighter skin-type individuals are often more aware of their skin because of their increased risk of skin cancer, darker-skin individuals may not be quite as vigilant.” To help catch these acral lentiginous melanomas early, everyone must be aware of the risk of melanoma on the hands, feet, and around and under the nails.
Skin cancer treatments include surgery, topical chemotherapy
Each year, more than 5 million cases of skin cancer are identified, with more than 198,000 of those cases projected to be diagnosed as melanomas in 2022. Almost 100,000 will be identified as invasive melanomas, while the other 98,000 as in situ melanomas. In situ melanomas are not invasive and are confined to the top of the skin and have no propensity to spread. Thus these in situ melanomas can be effectively cured with surgical removal. Many invasive melanomas may also be cured with surgery. However, some invasive melanomas may have more concerning features or may have already spread to other parts of the body at the time of diagnosis. These more concerning melanomas, besides surgical removal, may also require sentinel lymph node biopsy and possibly systemic therapy or other advanced therapy to target the melanoma cells.
The remaining cases of the more than 5 million skin cancers are mostly keratinocyte carcinomas, but “cutaneous squamous cell and basal cell carcinomas are not reportable cancers; therefore, we don’t have solid numbers on cases. Anywhere between 20 and 30% of keratinocyte cancers diagnosed are squamous cell carcinomas. The rest are basal cell carcinomas,” Dr. Paragh says. These cancers are often found in “cosmetically sensitive areas,” where surgical treatment can be emotionally stressful.
Check yourself for skin cancer
Find out how to perform a skin self-exam to check yourself for anything unusual.
Learn MoreMost keratinocyte carcinomas are removed by surgery; however, some early and low-risk non-melanoma skin cancers can be treated by topical chemotherapy, topical immunotherapy, or photodynamic therapy. Some keratinocyte carcinomas can metastasize. Although large and deep SCCs spread relatively frequently, the distant spread is seldom seen in BCCs. Even when keratinocyte carcinomas spread, targeted therapy, chemotherapy and immunotherapy offer hope for patients.
Dr. Paragh stresses that it’s essential for people to understand their personal risk for developing skin cancer, including knowing their family history. “If parents and grandparents talk to their children and grandchildren and tell them what they faced by not being careful with their skin, I think the kids will listen more and be more likely to take precautions early to help prevent skin cancer.” Understanding our risk can also help us better understand what to look for during self-skin checks and will help determine whether one needs regular dermatology skin check follow-ups to diagnose concerning lesions earlier.