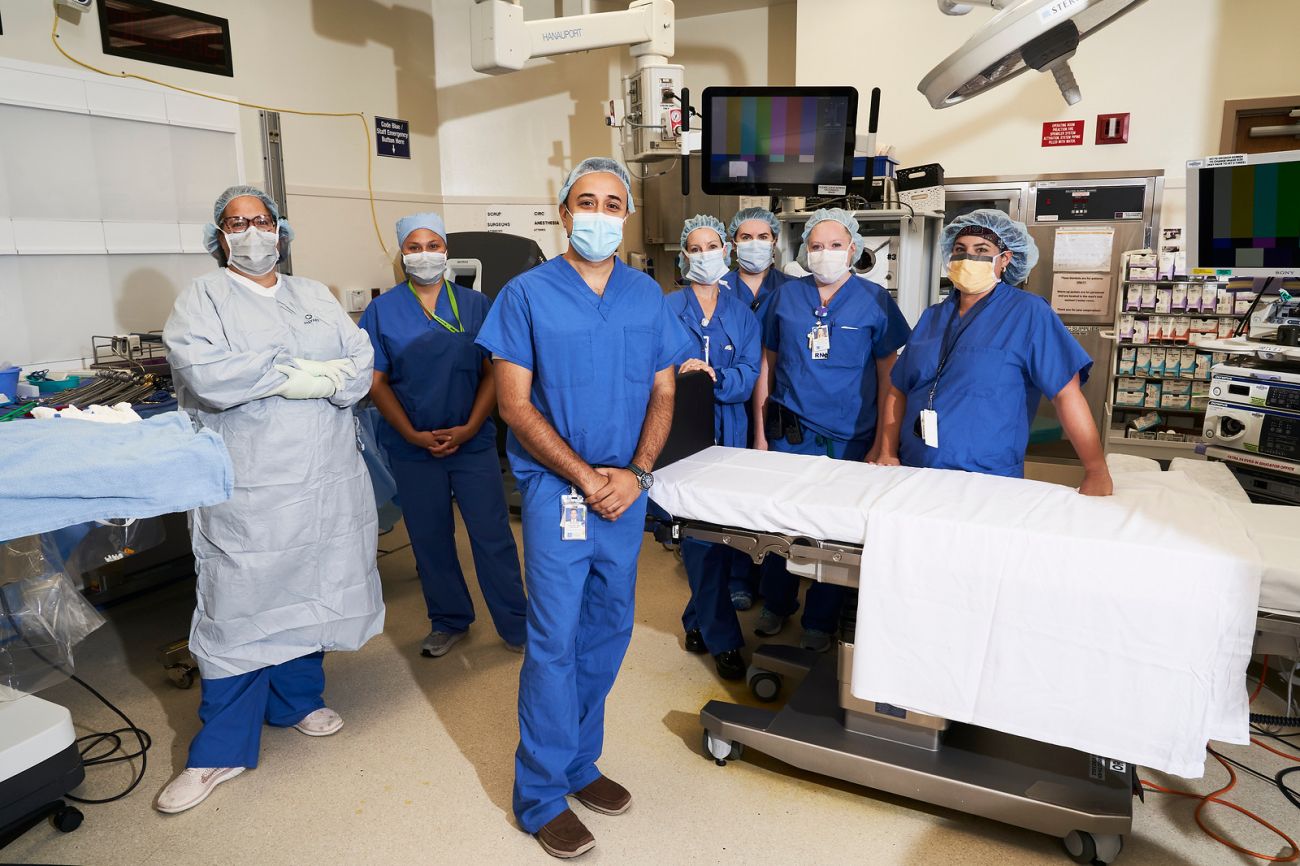
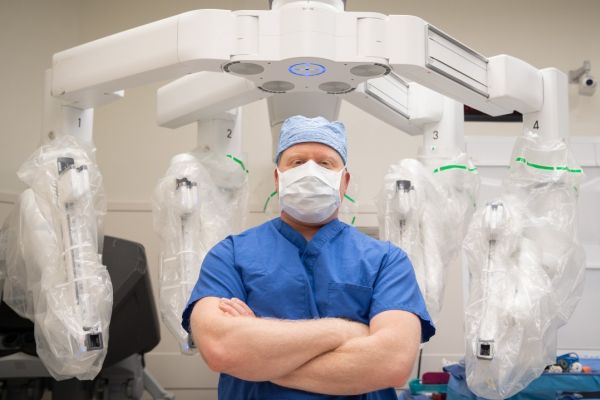
Our surgeons specialize in performing operations specifically for cancer — to treat it, diagnose it, and even prevent it from developing in the first place.
Surgery is a primary treatment for many patients and many types of solid tumor cancers. But it is often only part of the treatment plan. Whether you need surgery, and what type is determined in collaboration with other cancer specialists — medical oncologists and radiation oncologists, as well as pathologists, diagnostic radiologists and other specialists.
This multidisciplinary expertise ensures you get the right procedure at the right time in your treatment plan.
Types of cancer surgery
Roswell Park performs many operations using minimally invasive approaches such as robotic, endoscopic, bronchoscopic, endo-nasal procedures and more. Our ability to perform these advanced procedures means patients typically have a speedier recovery, less pain, fewer complications, shorter hospital stays and can start other parts of their treatment plan, sooner.
In addition, our teams aim to preserve your function and quality of life for years to come and perform breast-conserving, organ-sparing, nerve-sparing, limb-sparing, fertility-sparing and other complex procedures to limit impact on your well-being.
Highlights of our capabilities
Robotic surgery is now the standard for many procedures at Roswell Park, offering patients a precise, less invasive option with faster recovery times. We use this advanced technology for a wide range of cancers, including complex surgeries that few centers can perform, like robotic pancreas surgery and transanal surgery for colorectal cancer.
With decades of experience and a high volume of robotic procedures each year, our surgeons are not only experts in the field, they also train other doctors from around the world in these advanced techniques.
This specialized type of minimally invasive thoracic surgery offers many benefits to patients. Nationally, only 20-30% of lung surgeries use the VATS approach, but at Roswell Park, the rate of using VATS is as high as 90 percent. Roswell Park is a world leader in the number of VATS procedures for removal of a lung.
This advanced procedure requires unique expertise and can be an effective treatment for patients with cancers that have spread in the abdomen, such as primary peritoneal, appendiceal, ovarian, colorectal and other gastrointestinal cancers. First, cytoreductive surgery aims to remove all visible tumor in the abdomen. Then, heated, high-dose chemotherapy drugs are delivered directly to the abdomen.
Most neurosurgeons treat a broad range of neurological conditions and see very few brain and spine tumors. At Roswell Park, our neurosurgeons focus on tumors, malignant and benign, offering a range of procedures, such as awake craniotomy, endo-nasal skull base surgery, and a level of tumor expertise unrivaled in the region. With these critical tumors, your first treatment, typically surgery offers your best chance for outcome success. Make sure it’s the right one for you.
Our plastic & reconstructive surgeons use advanced microsurgery techniques to repair and restore tissue and structures, transfer skin, fat, muscle, and other tissue, and reestablish blood flow and nerve function to repaired areas.
We aim to fix what cancer took away. We provide highly specialized procedures to promote your healing, restore your function and appearance, improve scar deformities, eliminate the need for prostheses and improve your quality of life.
Why Roswell Park for cancer surgery
- If you have cancer, you need the very best surgical approaches today, and the simple truth is that these are not available at all hospitals or from all oncologists. They are found only at National Cancer Institute-designated centers. As one of the nation’s elite comprehensive cancer centers, we offer the latest technological advances and state-of-the-art facilities.
- Research shows more surgical experience translates into better patient outcomes. Our physicians have experience successfully treating a high number of patients with specific, or even rare types of cancer. Roswell Park doctors have more experience than those who see a small number of cancer patients each year and who don’t specialize in one cancer type.
- We provide a full menu of services — all in one location — for diagnosing and treating cancer, but also for helping survivors live healthy lives after treatment has ended. We offer services such as pain management, physical therapy, occupational therapy and many more to help speed up your recovery.
- For complex tumors, Intraoperative radiation therapy (IORT) delivers radiation in the operating room to the surgical margins immediately after the surgeon removes the cancer. This treatment kills potential microscopic disease at the surgical margin and is especially beneficial when tumors are next to a blood vessel and the surgeon cannot take any more tissue.