This is the second of two articles about Roswell Park’s new Chemotherapy Education Pathway. Part 1 appeared in our September issue.
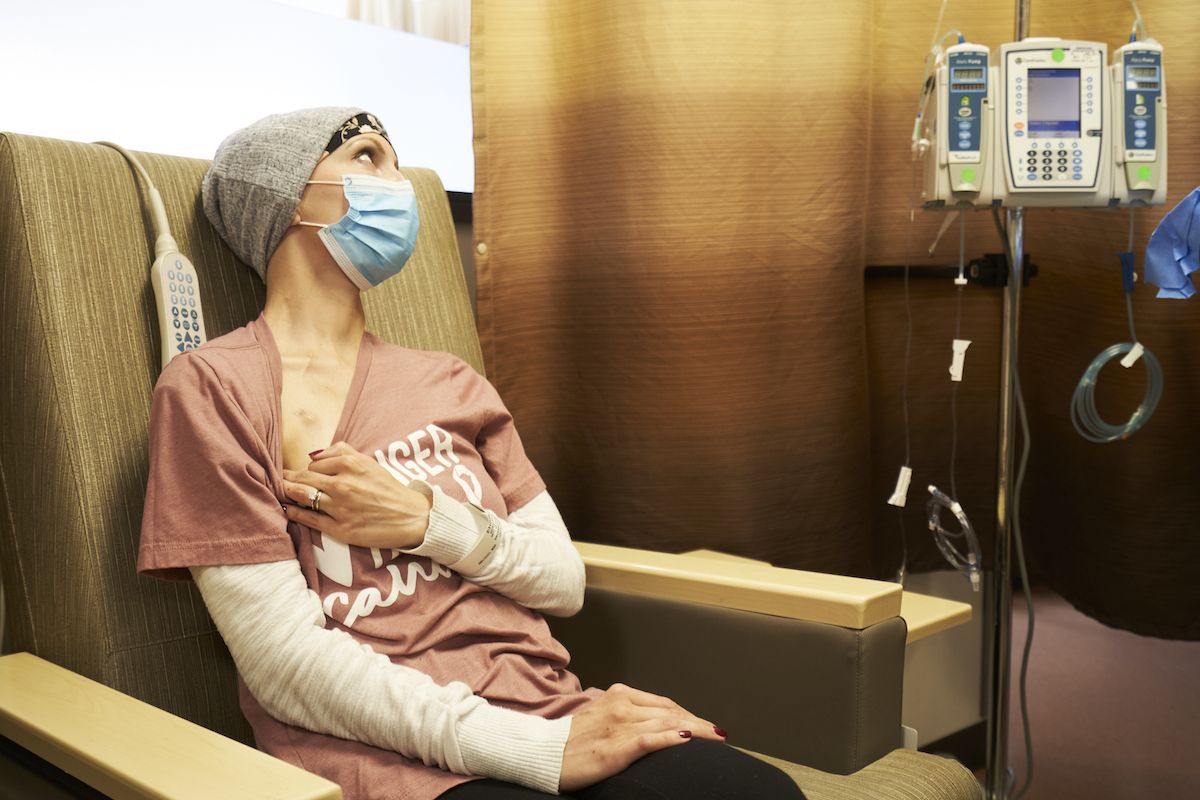
Four months ago, Christina Rauber was in “shell shock — speechless” after learning she had stage 2 breast cancer and would need to undergo six cycles of chemotherapy, followed by surgery and additional targeted therapy.
“I couldn’t believe I would have to endure this,” says the Rochester resident. “I have two kids, I have my husband, and I’m only 30. I was caught off guard.
“But then I thought to myself, Well, this is what I’ve got to do.”
Christina has now completed five of her six chemotherapy treatments in Roswell Park’s Chemotherapy & Infusion Center. She has experienced side effects along the way, but thanks to the new Chemotherapy Education Pathway, she was better equipped ahead of treatment. Knowing what might happen and how to deal with it has made the experience easier.
Chemo 101
On the day she found out that chemotherapy would be part of her treatment plan, she met briefly with her medical oncologist, Ellis Levine, MD, Chief of Breast Medicine at Roswell Park; Christina Matthews, PharmD, BCOP, a Clinical Pharmacist Specialist in the Breast Clinic; and medical fellow Maithreyi Sarma, MD. “They gave me a briefing: ‘During the first two weeks, you’re not going to feel normal. Days three, four and five are probably going to be your roughest. The third week will be your most “normal” week before you have to start all over again.’
“They also gave me a list of all my medications and handouts for me to read at home. I had an idea of what I’d be going through, and I knew I’d be getting a phone call later in the week to go even more in depth as to what each medication does.”
In the past, patients received their chemotherapy education during the same clinic visit when they were told they needed chemotherapy. But patients reported that they were overwhelmed by information overload; sometimes they didn’t fully understand or remember everything they needed to know.
Under the Chemotherapy Education Pathway, first they receive printed materials during a clinic visit. They have time to review and process the information at home for a few days and to think of questions they’d like to ask before speaking with a clinical pharmacist in a longer conversation, which can last from 45 minutes to an hour.
The packet of materials includes “Preparing for Drug Therapy,” a one-page sheet that explains what they will learn about during a visit with their oncologist and what their pharmacist will explain during a one-on-one teaching session. Patients on IV chemotherapy will have an orientation to Roswell Park's Chemotherapy & Infusion Center, either in person in the Resource Center for Patients and Families or via online videos. Because patients on oral chemotherapy are not treated in the Chemotherapy & Infusion Center, their information packets are different.
Patients also receive a copy of “Taking the Lead: What You Can Do to Live Well During Drug Therapy.” Designed as a handy reference to use throughout treatment, it covers many topics, including nutrition, exercise, sleep, relaxation techniques, body image and hair loss, sexuality and fertility, preventing infection, precautions to take at home, and medical marijuana, plus a list of important phone numbers.
Christina says having a few days between the time she received the materials and got a follow-up call from the pharmacist gave her time to absorb what she had read. “I was able to prep myself before being on the phone; that was very helpful. I was able to ask questions I had already written down.” She finds it reassuring to be able to go back and look at the printed materials again when she has questions about side effects or other issues.
First Stop: Resource Center for Patients and Families
Before starting her treatments, Christina stopped in at the Resource Center for Patients and Families, where she learned about hair loss caused by some types of chemotherapy. She selected a wig from the Wig & Hat Boutique and picked up a chemotherapy and infusion support kit. Patient Education Facilitator Martha Hickey says contents of the kit vary depending on the needs of the individual patient, but patients like Christina who will undergo IV chemotherapy receive a "port pillow" to prevent seatbelts from rubbing against the chest ports where they will get their infusions. In addition to a wig, all patients may choose a hat and sleep cap, a cookbook that includes suggestions about what to eat on the day of chemotherapy, and "goodies" from various donors, which may include a blanket or shawl, water bottle, mints, journal and pen, makeup samples or other items.
The Resource Center staff “were so, so kind and helpful,” says Christina. When they advised her to brush and floss regularly to prevent oral infection, she burst out laughing. “I’m a dental hygienist, so I said, ‘Yes, that will definitely be happening.’”
Never miss another Cancer Talk blog!
Sign up to receive our monthly Cancer Talk e-newsletter.
Sign up!A few days later, it was time for her chemotherapy education session with Christina Matthews. “I really enjoyed the phone conversation,” says Christina Rauber. “It covered every base. Christina gave me a ton of information and never made me feel stupid for asking about things. I really appreciated that.”
Since her treatment began, Christina has experienced many of the side effects described for her during her chemotherapy education:
- Nausea. “I’ve gotten it maybe five times. I was lucky; it was quick and easy, maybe 10 minutes of it, and then I felt better.”
- Neuropathy. “I sometimes get it in my feet and hands. It’s not long-lasting, but I have only one more hard-core treatment left, so hopefully that will lessen.”
- Mouth sores. “I got them only once, after my first treatment.”
- Bone pain. “They warned me about the bone pain that can happen after having the Neulasta®, and to take Zyrtec® or Claritin®. That helped a ton.”
- Changes in taste. “Another thing is the zonking of the taste buds, when you can’t taste certain things. That hasn’t been too bad; it was more in the beginning versus now.” She was advised to try a milder diet, which helped.
- Hemorrhoids. Hemorrhoids can be relieved with Tucks® medicated wipes, witch hazel and certain types of Preparation H® lotions.
- Dry mouth. Although Christina does experience dry mouth, “it’s not every day.” As a dental hygienist, she was already familiar with ways to deal with it. “I like Biotène® gel specifically. It gives longer-lasting relief than the mouthwash.”
She continues to keep in close touch with Christina Matthews. “We message back and forth and talk if I’m having an issue with something that’s not responding to medication or a topical gel.” When they’re not in direct contact, “In my head I replay Christina’s voice and think, OK, this makes sense. It’s a side effect — that’s what’s happening to me right now.
“You’re always going to feel worried, because you don’t know what your body’s going to do. But now I feel more confident. I want to get all the information I can to get through this and be educated the best I can.”
Editor’s Note: Cancer patient outcomes and experiences may vary, even for those with the same type of cancer. An individual patient’s story should not be used as a prediction of how another patient will respond to treatment. Roswell Park is transparent about the survival rates of our patients as compared to national standards, and provides this information, when available, within the cancer type sections of this website.