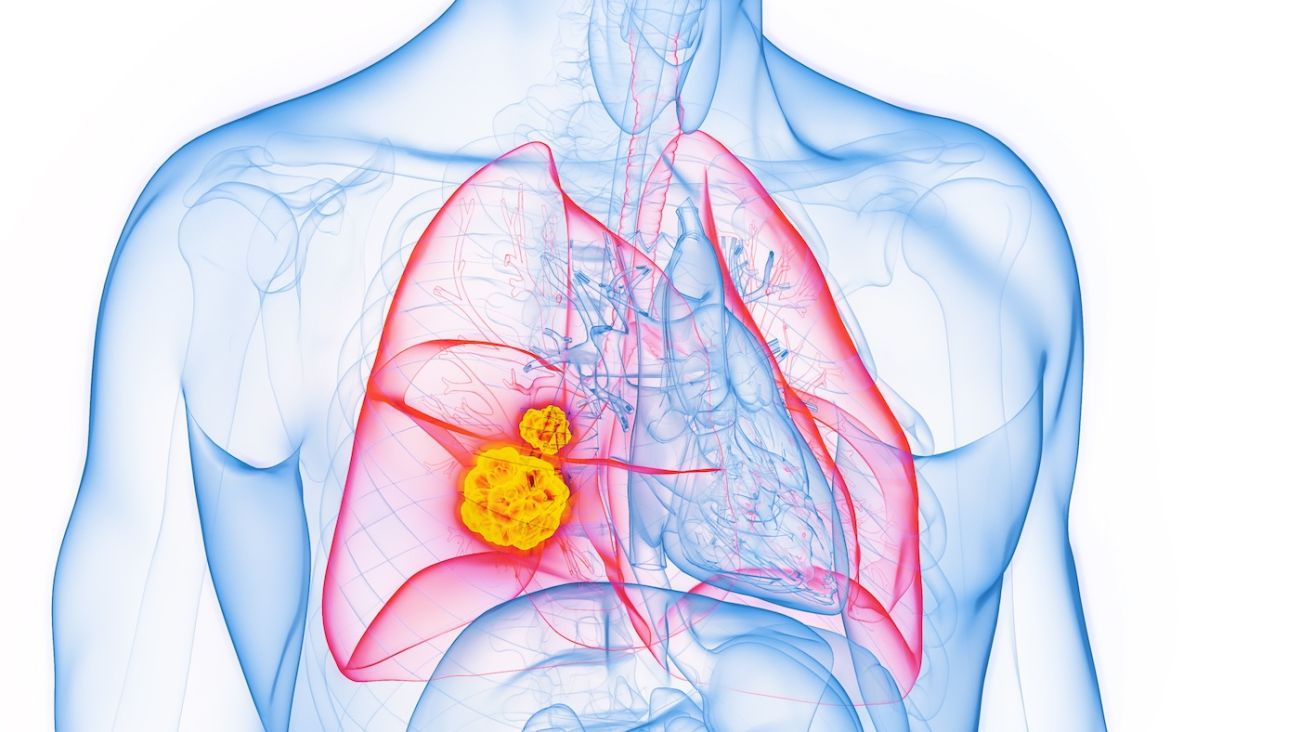
Although many are benign, these spots in the lung may be the first warning sign of cancer. Their evaluation requires expertise to ensure an accurate answer.
Lung nodules — abnormal growths in the lung — may show up on X-rays and CT scans as a spot or shadow. While most are benign and are not cancer, they do need to be investigated to rule out cancer and monitored for growth or other worrisome changes that may indicate cancer.
Nodules appear on a scan as a dense spot that looks different than surrounding tissue, explains interventional pulmonologist Nathaniel Ivanick, MD, of Roswell Park Comprehensive Cancer Center. “Some are cancerous; many are not,” he says.
Some nodules can be caused by previous lung infections or inflammation, “like scar tissue,” he says. Other infections may come from inhaling a fungus, though that is less common in the northeast than in other parts of the country like the southwest and California. Rheumatoid arthritis and other autoimmune diseases can cause nodules that look like cancer, he says, as can exposure to dust or chemicals. Some may be metastatic spread of cancer from other parts of the body. “The older you get, the more likely you are to have nodules,” he says. “Risk goes up by decade.”
Current and previous smokers are more likely to have lung nodules, as are people exposed to radon, secondhand smoke or environmental pollutants. “Nodules in smokers are more concerning because they are more likely to be cancer,” Dr. Ivanick says. “The lung cancer rate for any given nodule is 1.5%, however it is detected. Among smokers it is more like 33%.”
How nodules are detected
Nodules are typically found in one of two ways. “The first is by looking for them in a high-risk person having a screening, such as smokers between 50 and 80 who didn’t quit smoking long ago enough,” he says.
Annual lung cancer screening with a low-dose CT scan is recommended for people with the following three factors:
- Ages 50 to 80
- Have a 20 pack/year smoking history (such as smoking a pack a day for 20 years or two packs a day for 10 years)
- Currently smokes or quit within the past 15 years
The other group is patients in which a nodule was found while looking for something else — for instance, someone in a car accident got a CT scan, and it was found then. We track these nodules using slightly different guidelines.
Getting a biopsy of a lung nodule
If a nodule is deemed very suspicious — about 2% of cases, says Dr. Ivanick — the doctor might take a tissue sample for biopsy. A nodule might be suspicious due to a large size, if it grows over time (as seen on serial CT scans) or if it has features such as spikes or points on the surface. Doctors may take a biopsy either with a needle biopsy while getting a CT scan or with robotic navigational bronchoscopy. “We were the first hospital in New York to use this platform, which uses an earlier CT scan like GPS to help the robot find the best pathway to take,” he says. “Airways branch so many times, we need a roadmap to get us out to the right spot.”
Each modality has advantages and disadvantages, which the doctor discusses with the patient when choosing the right option. A third option is to take a sample surgically, particularly if the nodule is close to the edge of the lung and more easily reached. “If the risk is high enough and we’re pretty sure it’s cancer, the surgeon may offer different approaches, including wedge resection or lobectomy,” he says.
If scans reveal that lymph nodes are impacted, that “can shift the level of concern toward biopsy rather than not,” Dr. Ivanick adds. “In part it’s the clinician’s feeling about these cases, based on conversations with patients and their preference. Some want action taken earlier, some don’t want to consider anything until surgery is necessary. We take the comfort level of the patient into account.”
Lung cancer screening made easy
Eddy — Early Detection Driven to You — is lung cancer screening on wheels. Eddy’s goal? Make it easy for more people in New York State to get screened for lung cancer.
Do all lung nodules need to be evaluated?
Not always, but it depends on how and why the nodule was found, the patient’s age and health history and the size and type of nodule. If the patient is that hypothetical person in a car accident who was found to have a nodule, the nodule is small and he or she has no history of smoking, yearly follow-up scans over several years may be all that is required. A larger nodule or one with certain physical characteristics may require more frequent scanning. A nodule in the upper lobe of the lung is more likely cancer.
If the biopsy shows signs of underlying infection, that could get treated. If it’s a rheumatoid nodule, the care team may initiate treatment of this systemic disease. “If there are no other symptoms, no treatment may be needed,” he says. However, if the patient is a smoker or former smoker, a nodule requires more careful monitoring.
Depending on its size, location, characteristics and change over time, the doctor may follow several courses of action. “It’s always dictated by the underlying diagnosis,” he concludes.
Should you see an oncologist for lung nodules?
Whatever the circumstances, patients should come to a comprehensive center like Roswell Park for monitoring of their lung nodules. “There is good data to suggest that getting lung cancer screening and treatment at a place with a centralized screening program and expert diagnostic team helps patients get the best outcomes,” Dr. Ivanick says. In addition, “Roswell Park is lucky to have many experts in the field, so there is a lot of talk behind the scenes. If a patient is seeing me, for instance, I know to lean on colleagues in other specialties here. They are just a phone call away. That makes Roswell Park pretty special.”
Though there are lots of ways to treat lung cancer, “we are at the forefront of developing even more of them — even non-surgical techniques. Even if it’s not early-stage cancer, we run clinical trials of the latest approaches. And with early screening, we see more early diagnoses, which make more treatment options possible.”