Roswell Park offers effective treatments for this complex condition.
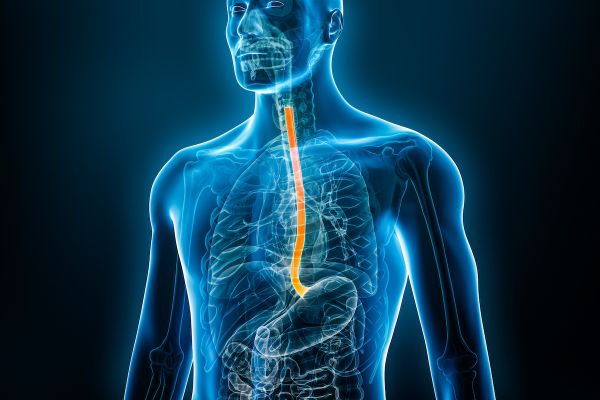
Achalasia is a rare swallowing disorder in which the esophagus loses the ability to propel food and liquids into the stomach. As a result, food gets stuck in the esophagus, leading to regurgitation of food and often chest pain.
Normally, when you swallow food and beverages, wave-like contractions called peristalsis propel what you’ve swallowed down your esophagus. Then, a juncture of muscle where the esophagus and stomach meet — called the lower esophageal sphincter (LES) — relaxes, allowing the food to enter the stomach. With achalasia, both these processes, peristalsis and relaxing of the sphincter, don’t work properly.
What causes achalasia?
“The exact cause of achalasia is not completely understood, but it involves significant disruption to the nerve cells in the esophagus, specifically those that help control the relaxation and opening of the LES,” says K. Patrick Seastedt, MD, a thoracic surgeon with Roswell Park Comprehensive Cancer Center.
Possible causes of this nerve damage include an autoimmune response, where the body's immune system mistakenly attacks the nerve cells in the esophagus. “Some researchers believe that certain viral infections could trigger an autoimmune response that leads to the degradation of these nerves,” Dr. Seastedt explains.
Symptoms of achalasia
Achalasia can happen at any age but typically occurs in individuals over age 50. It is sometimes mistaken for gastroesophageal reflux disease (GERD). Recognizing the symptoms of achalasia is crucial because early detection can lead to more effective management. Here are the key signs to watch out for:
- Difficulty swallowing (dysphagia) or feeling as if food or liquids are stuck in your chest.
- Regurgitating undigested food without the typical forceful contractions of vomiting and often when lying down or bending over.
- Chest pain that can vary from mild discomfort to severe that mimics heart pain. The pain stems from the esophagus attempting to push food through the restricted LES.
- Weight loss. Ongoing difficulties with eating and the fear of painful swallowing can lead to significant and unintentional weight loss.
- Aspiration. In severe cases, food or liquid may accidentally enter the lungs, leading to coughing or even serious lung infections like aspiration pneumonia. Patients typically experience coughing and/or choking during eating.
Patients also may experience symptoms that mimic GERD, such as heartburn and chest pain in addition to regurgitation.
Switch to Roswell Park
If you are receiving treatment for a non-malignant disease, you may benefit from the specialized treatment options an NCI-designated cancer center provides.
Treatments for achalasia
"There are many treatment options for achalasia. Each has its benefits and risks, and the choice often depends on individual factors that include the severity of the condition, the patient's overall health and personal preferences,” says Dr. Seastedt. Making lifestyle adjustments, such as eating slowly and choosing soft foods, can help manage symptoms. Elevating your head during sleep can help to prevent regurgitation and aspiration, especially at night.
In addition, some medications such as calcium channel blockers and nitrates can temporarily relieve symptoms by lowering the pressure in the LES, making it easier for food to pass into the stomach. Botulinum toxin (Botox) injections directly into the LES also can temporarily relieve symptoms by preventing the muscles from contracting normally, thus reducing the pressure and allowing food to pass more easily.
Roswell Park offers additional options that provide a longer-term solution to treat this complex condition, including:
- Pneumatic (balloon) dilation, in which a balloon is inserted through the LES during an endoscopy. The balloon is then inflated to forcibly widen the opening.
- Peroral endoscopic myotomy (POEM) is a minimally invasive procedure which uses an endoscope to loosen LES muscles to permanently reduce LES pressure.
- Heller myotomy is a surgical procedure that involves cutting muscles accessed from the outside of the esophagus.
"POEM had advantages over laparoscopic Heller myotomy because POEM is performed entirely through the mouth, minimizing recovery time and reducing the risks associated with invasive surgery such as the Heller myotomy,” explains Dr. Seastedt. “Everything is done using the endoscope, without incisions on the outside of the body.
The POEM procedure targets the root cause of achalasia: the inability of the lower esophageal sphincter to open properly. The procedure has shown high success rates in reducing achalasia symptoms and is particularly effective in managing all types of the condition.
Why Roswell Park for achalasia treatment?
While POEM is a safe and effective treatment for most patients with achalasia, it is a specialized procedure that should be performed by an experienced thoracic surgeon or gastroenterologist trained in advanced endoscopic techniques. Although achalasia is not a form of cancer, the treatment for this complex esophageal condition benefits significantly from the high level of expertise and interdisciplinary care typically found at specialized medical centers like NCI-designated Roswell Park. “Roswell Park’s thoracic surgeons are skilled in advanced diagnostic and treatment techniques that are crucial for managing achalasia effectively. Our state-of-the-art diagnostic tools that provide detailed images and functional tests of the esophagus, ensuring that each patient receives a precise diagnosis.”
Beyond the physical treatment of achalasia, Roswell Park is committed to the overall well-being of its patients. Support services, including nutrition guidance, physical therapy and psychological support, are part of our comprehensive care package. “As a leading research institution, Roswell Park is at the forefront of the latest medical research and treatment innovations. Patients benefit from access to new therapies and techniques that might not be available elsewhere,” says Dr. Seastedt.