Roswell Park offers new approach for lung condition
A minimally invasive procedure called endobronchial valve therapy is a nonsurgical way to redirect air from a poorly functioning part of the lung to a healthier part, resulting in easier and better breathing. Roswell Park has used endobronchial valve therapy for years, typically to treat airway leaks that may persist after lung cancer surgery or a biopsy. Now the procedure is offered to people with severe emphysema.
Roswell Park is the only facility in Western New York that has both the technology and the expertise required to offer the treatment. “We were getting calls from physicians in the community asking if we could help their patients,” says thoracic surgeon Elisabeth Dexter, MD, FACS, FCCP. “Yes, we can.”
What is emphysema?
Emphysema is a type of chronic obstructive pulmonary disease (COPD) in which lung damage (typically from smoking) causes the lungs’ air sacs to lose their elasticity and ability to push air out when exhaling. With healthy lungs, when a person inhales, the air sacs inflate and exchange inhaled oxygen for carbon dioxide, which is exhaled. But in people with emphysema, the air sacs cannot make the exchange or push carbon dioxide out of the lungs. As a result, the sacs remain partially inflated, reducing the ability to exhale completely and inhale oxygen effectively. The constant shortness of breath and struggle to breathe take a toll on mobility and quality of life.
How do the valves work?
One treatment for emphysema, lung volume reduction surgery, is an operation to remove a lung, lobe or section of the lung. With endobronchial valve therapy, lung volume reduction can be achieved without removing any lung tissue. The valves block inhaled air from diseased portions of the lungs and redirect it to healthier portions of the lungs instead. Over time, the blocked portions of the lungs shrink, allowing the healthy parts to take over the work.
“Lung function, physical function and stamina improve, and patients can be more physically active and will feel better overall,” says interventional pulmonologist Nathaniel Ivanick, MD. “Some can come off supplemental oxygen. There’s no cure for emphysema, but this is a way for the lungs to return to a less diseased state where they’re functioning better.”
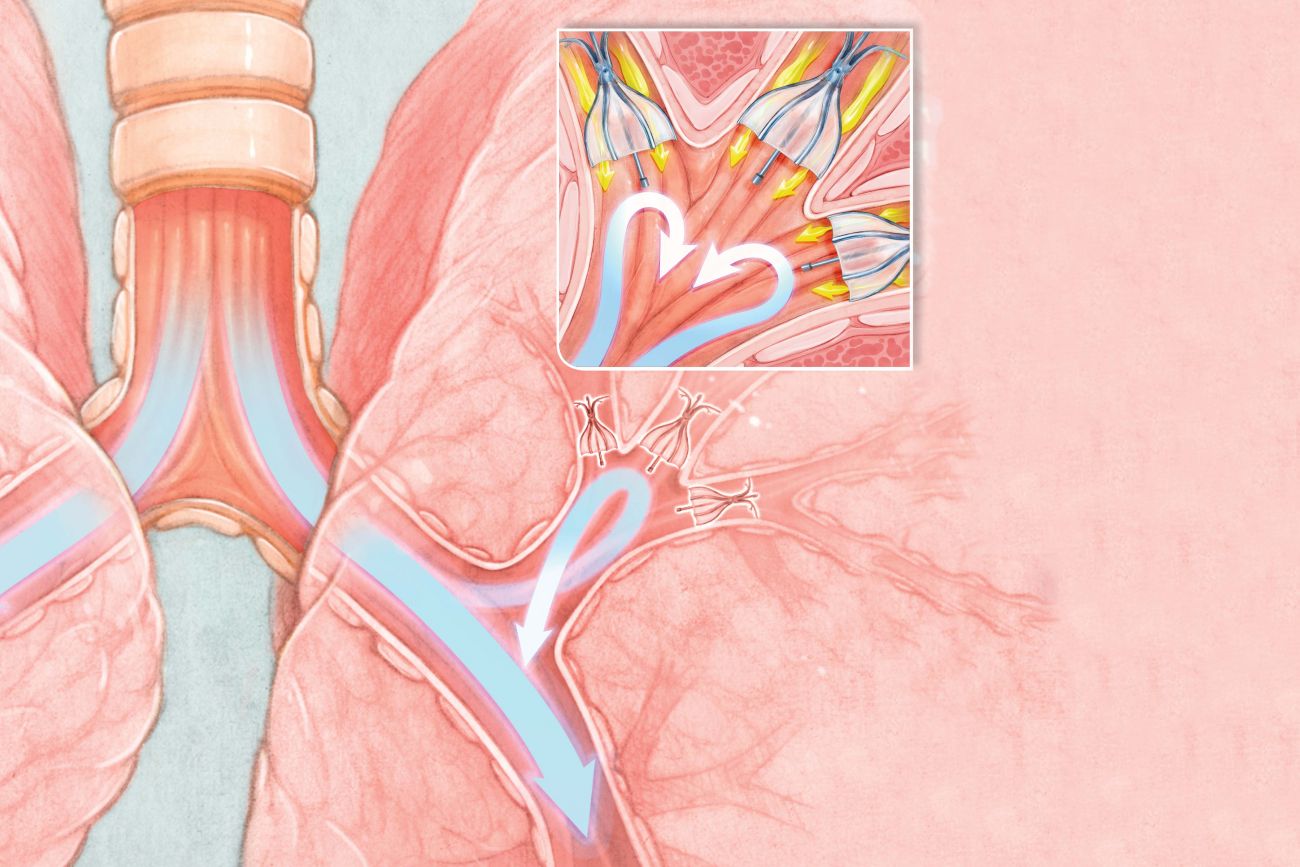
To reach the lungs, a long, tube-like instrument called a bronchoscope is inserted through the mouth and into the lungs. With the bronchoscope, a thoracic surgeon or interventional pulmonologist places three to five tiny valves, slightly larger than a pencil eraser, into the airways (bronchi) that lead to the nonfunctioning air sacs. Two different types of valves may be considered for the procedure. One type resembles a tiny upside-down umbrella, while the other is like a funnel, but they have the same purpose: the valve captures inhaled air and redirects it to a different airway. At the same time, air already in the sacs can exit.
“The valves are able to accomplish what was previously done with surgery, actually removing the section or lobe of lung,” explains Dr. Dexter. “That surgery has a long recovery time and high morbidity and mortality. Not only is valve therapy less invasive, but it can be reversed. We can simply remove the valves if the patient does not do well with them.”
Who is eligible?
These valves work best in specific patients. Patients must go through an evaluation process that includes pulmonary function testing, CT scan, ventilation perfusion scan and more. “The emphysema has to be significant enough that the patient will benefit from the treatment,” says Dr. Ivanick, “but the patient must have quit smoking and cannot have excess mucus or cancer. If the person has cancer, first and foremost, we treat the cancer.”
One valve type works best in patients whose emphysema is concentrated in one area or side of the lung. Another valve type is appropriate for patients who have emphysema throughout the lungs. “Not all people with emphysema will be eligible for valve therapy,” says Dr. Ivanick. “But here we have six thoracic surgeons and an interventional pulmonologist. We have the resources to offer other options."
Become a Patient
Are you eligible for this treatment? Make an appointment by calling 1-800-ROSWELL (1-800-767-9355) or filling out our online form.