Learning about the road map of your circulatory system
It’s more common to have blood taken from a vein than to have medications infused into one. So why doesn’t the nurse who gives you chemotherapy use the same vein as the phlebotomist who draws your blood?
Veins & Arteries: Apples & Oranges
Your heart and blood vessels form a closed loop that keeps blood flowing through your body, delivering oxygen to your cells and carrying away waste products. The blood vessels — arteries and veins — are different from each other.
Arteries perform the following functions:
- Carry blood away from the heart. In most cases, blood in an artery has a high level of oxygen and few waste products.
- Have thick (muscular) walls, because the blood being pumped from the heart puts great pressure on them.
- Have internal pressure strong enough to fight gravity and push blood up to your brain.
Veins perform the following functions:
- Carry blood toward the heart. In most cases, blood in a vein has a low level of oxygen and contains more waste products.
- Have thinner walls and lower pressure on the inside. The lower pressure can make it more difficult for the blood to return to the heart, so veins have one-way valves in them to prevent blood from pooling or flowing backward because of gravity or other forces.
- Have a wider diameter than arteries and can hold more blood. At any given time, most of our blood is in our veins. This extra blood means that losing small amounts of blood doesn’t harm us.
Because of their thinner walls, larger diameters, larger blood volume, and lower pressure, veins are the preferred access point for drawing blood or giving fluids and medications.
Drawing Blood vs. Giving Medications
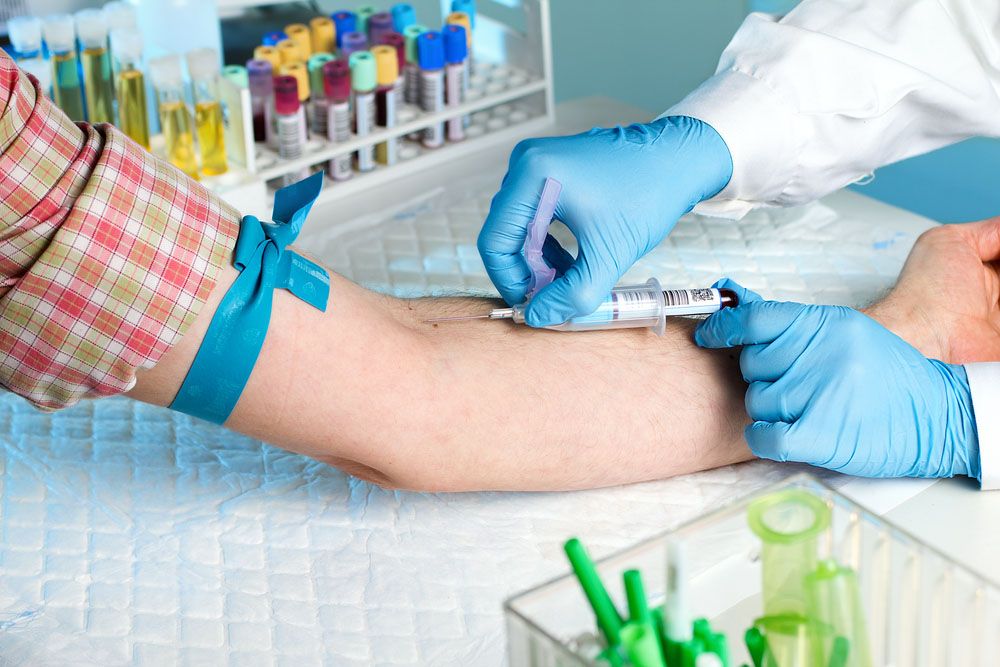
When drawing blood, the phlebotomist chooses a vein that will allow quick, easy access; has good blood flow; and will cause the least discomfort to the patient. Blood is often drawn from a vein near the crease of the elbow.
When giving medication, a nurse must find a vein that is large, smooth, and pliable. (Chemo can make veins less elastic and smaller in size.) The nurse will start looking in the hand and move up the arm. (Starting lower helps save higher access sites for the future.) During this process, the nurse also needs to think about whether the medication will irritate the vein, and how long the infusion will last.
These best practices are based on research and supported by professional organizations such as The Oncology Nursing Society (ONS). They specify both what should be done and what things to avoid — for example, using veins in the inner elbow (where blood draws commonly occur), the dominant arm, the inner and upper surfaces of the wrist, the legs, or areas at risk for complications (areas of pain, infection, inflammation, bruising, poor circulation, and those affected by previous medical procedures).