Experts vary on when to begin and which test is preferred, but just getting it done matters most
Cervical cancer screening has had a dramatic impact on preventing the development of cervical cancer and decreasing deaths due to this disease. Routine cervical screening — with cervical cytology (commonly known as the Pap test) and/or HPV testing — detects precancerous conditions before cancer develops, opening an important window of opportunity for early treatment or prevention of the disease altogether.
About the cervical cancer screening tests
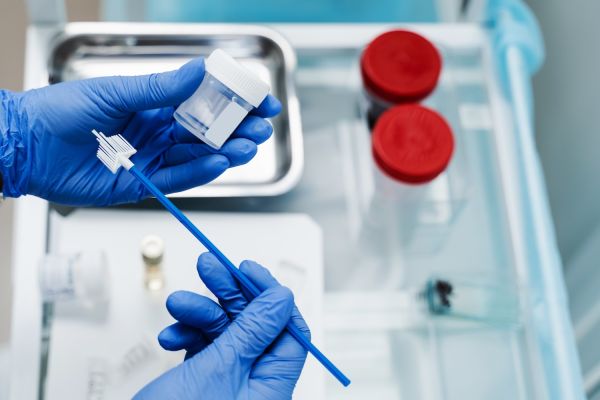
Currently, two tests are performed as a part of cervical cancer screening, and they are performed in the same way in your doctor’s office — by collecting a sample of cells from the cervix with a scraper or brush. The tests are fast, easy and part of routine well-woman healthcare visits.
Cervical cytology examines cervical cells for abnormal changes called cervical dysplasia, which could lead to cervical cancer. The HPV test examines cells for the presence of the human papillomavirus (HPV), which can lead to cervical cancer. (Performing both together is called the HPV/Pap cotest.)
When to begin cervical cancer screening
Current guidelines issued by the U.S. Preventive Services Task Force and other organizations recommend that patients begin cervical cancer screening at age 21 and undergo the Pap test every three years if results are normal. Beginning at age 30 and continuing to age 65, patients should undergo HPV/cervical cytology cotesting every five years if results are normal.
A history of abnormal results means you’ll undergo more frequent screening. Patients who have received the HPV vaccine still need cervical cancer screening, because the vaccine prevents infection with most — but not all — of the HPV strains most commonly associated with cancer.
New guidelines proposed
Last fall, the American Cancer Society revised their screening guidelines. They now recommend starting screening at age 25 instead of 21. They also recommend HPV testing as the primary screening test, with later cervical cytology if HPV infection is found. But why delay screening?
“When you look at all new cases of cervical cancer in the United States, patients aged 20 to 24 make up less than 1% of those cases, but their rate of transient HPV infections is very high,” says Roswell Park gynecologist oncologist Katherine LaVigne Mager, MD. “This means that you are going to be finding and treating a lot of abnormalities that have a very low likelihood of progressing on to cervical cancer.”
Simply put, this means that for most of these patients, the HPV infection clears up, the cell changes resolve and they are not at increased risk. Delaying the start of routine screening for four years could help to avoid unnecessary interventions.
Life has opened back up. Now it’s time to get back to health.
If you’ve waited to schedule your cancer screening, delayed your doctor’s appointments or are ignoring that lingering symptom that is just not right – now is the time to act.
Learn MoreIs the HPV test better than cervical cytology?
The HPV test is a newer method of testing compared to cervical cytology (Pap test), which has been around for decades. What’s most important in terms of your risk for developing cervical cancer is the HPV status, explains Dr. Mager. “As we have learned more about the relationship between HPV infection and the development of cervical cancer, it has become very clear that HPV status is very important. While there are some rare types of cervical cancer that are not associated with HPV infection, the vast majority are. If you have negative HPV testing, we know that the likelihood of you having abnormal cells on your cervical cytology is extremely low. HPV positivity or infection with a high-risk strain of HPV is what will increase your risk of the development of cervical cancer.”
The new guidelines aim to fine-tune the recommendations so that screening is more efficient and balances the benefits of screening with the risks of more interventions. While the American Cancer Society has proposed these guidelines, many national organizations have not yet changed their recommendations.
“National cervical cancer screening guidelines are still in a period of adjustment, so don’t be worried if your doctor is recommending screening starting at 21 or you are still having cervical cytology performed,” says Dr. Mager. “Both screening approaches are good, safe, reasonable and effective.”