How removal of your uterus affects risk for ovarian, uterine and other GYN cancers
Women undergo hysterectomy — surgical removal of the uterus (womb) — for many reasons other than cancer, such as uterine prolapse or to address heavy bleeding or pain from fibroids or endometriosis. Hysterectomy is the second most common surgery among women in the United States (childbirth by cesarean delivery is first), and as many as 600,000 undergo it each year. Among women age 50 and older in the United States, nearly 32% have had a hysterectomy. If you’re in this group, what does it mean for your cancer risk?
What did my hysterectomy include?
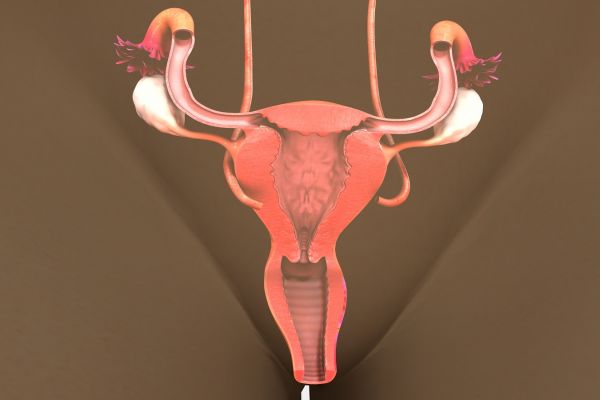
While your risk for developing uterine cancer is dramatically lowered by the surgery, your risk for other gynecologic cancers — such as ovarian — may not be, explains gynecologic oncologist Peter Frederick, MD, Clinical Chief of Gynecology at Roswell Park. It largely depends on what type of surgery you had in addition to your hysterectomy. In other words, were other structures — your ovaries, fallopian tubes, cervix — removed or left in place?
For example, a total hysterectomy removes the uterus and cervix. A partial hysterectomy (also called subtotal or supracervical) removes just the upper part of the uterus, leaving the cervix. Ovaries and fallopian tubes may or may not be removed along with the uterus and cervix. Even a radical hysterectomy — removing all of the uterus, cervix, upper part of the vagina and some surrounding tissue — may or may not remove the ovaries and fallopian tubes.
Ovarian cancer still possible after hysterectomy
In situations when the hysterectomy is done for benign (noncancerous) conditions, the ovaries may be left in place in order to retain important hormonal function and avoid sudden onset of menopause. If you still have your ovaries, your risk for ovarian cancer is reduced after a hysterectomy, but it is still present. For most women without a family history or other predisposition for ovarian cancer, this risk is very small (less than a 1 in 70 lifetime risk). New evidence suggests that many cases of ovarian cancer may actually begin in the fallopian tubes, so some women who elect to keep their ovaries decide to have their tubes removed to decrease that risk.
What's Your Cancer Risk?
Worried about your ovarian cancer risk? Take our Ovarian Cancer Risk Assessment.
For women at high risk for ovarian cancer who undergo risk-reducing surgery with removal of the ovaries and fallopian tubes (such as women with a BRCA mutation), the lifetime risk of ovarian cancer is dramatically reduced. Unfortunately, the risk of cancer is not completely eliminated, because peritoneal cancer (cancer arising from the inner lining of the abdominal cavity) may still occur. Peritoneal cancer is treated the same way as ovarian cancer.
Do I still need screenings?
Yes, women still need routine gynecological exams and cancer screenings. Most women (those at average risk) should have an annual gynecologic exam by their healthcare provider. In addition, women should have routine cervical cancer screenings until age 65. This means a Pap test every three to five years to detect precancerous changes in the cervix and an HPV test every five years to detect the presence of human papillomavirus, a cause of many cervical, vaginal, oral and head and neck cancers.
If you are at increased risk for a gynecological cancer due to your family’s cancer history, BRCA gene mutations or other genetic syndromes in your family, or you’re taking medications such as hormone replacement therapy or tamoxifen, your screening recommendations may be different. Be sure to update your family history and discuss these factors with your primary care physician.
In addition, tell your doctor about any persistent, new or unusual symptoms such as:
- Vaginal bleeding or discharge
- Pelvic or abdominal pain, pressure or bloating
- Pain during sex
- Difficulty eating
- Change in bowel movements
- Change in urinary habits, such as increased frequency and/or urgency or difficulty emptying your bladder
- Change in appetite
- Unexplained weight gain or weight loss
When it comes to gynecologic cancers, the good news is that your hysterectomy eliminates your risk for the most common diagnosis — uterine cancer — and reduces your risk for other cancers, such as ovarian, fallopian tube and peritoneal cancers. If your ovaries and fallopian tubes were also removed, then your risk for the most deadly gynecologic cancer, ovarian, is significantly reduced, too. Your risk for other gynecologic cancers, such as cervical, vulvar and vaginal cancer, can be reduced with regular exams and screenings.
Do You Need to be Screened?
Not sure which cancer screening tests you need now? Our Cancer Screening Center is open to everyone. You can schedule a cancer screening exam or take our screening and prevention questionnaire and we’ll provide the guidance you need.