With this advanced, minimally invasive procedure, Roswell Park treats brain tumors, disorders and metastatic lesions, providing an alternative option that spares patients from the side effects of whole-brain radiation.
What is Gamma Knife radiosurgery?
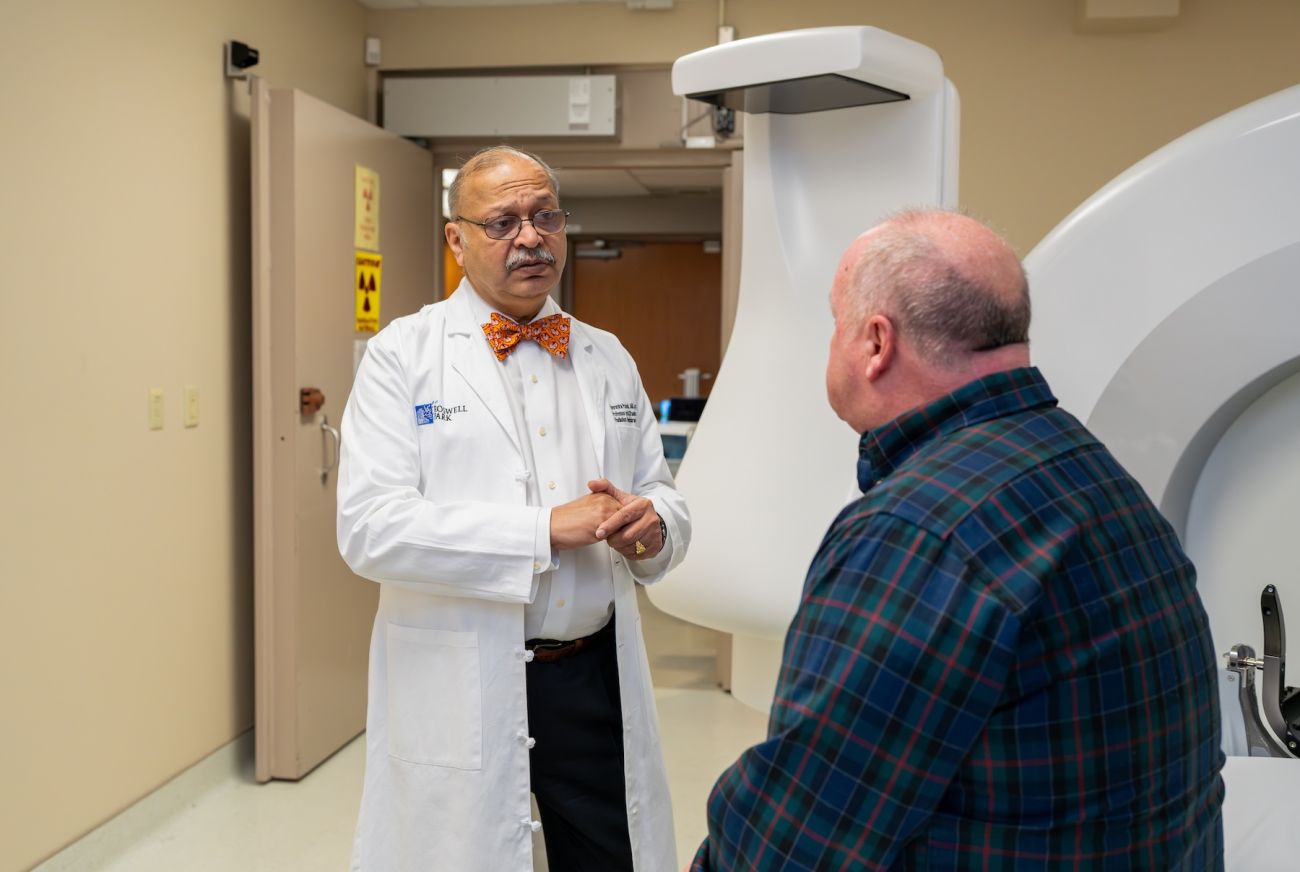
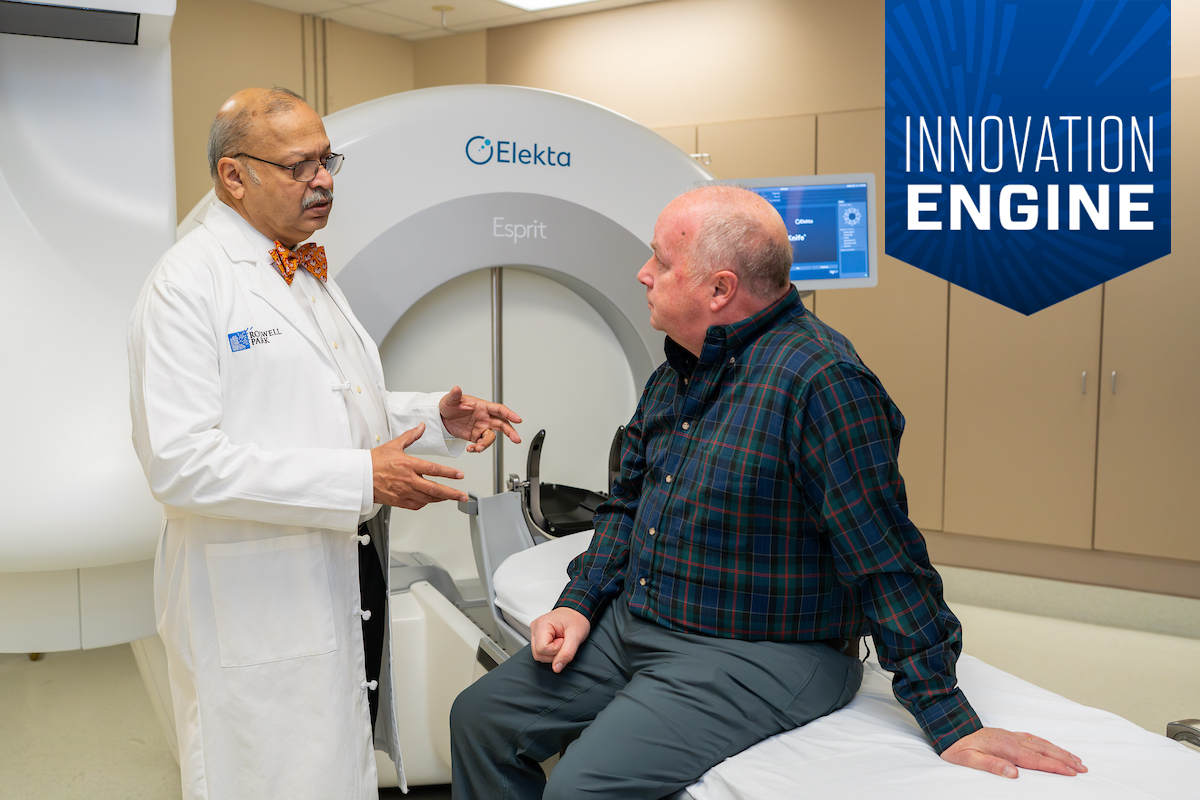
Gamma Knife radiosurgery isn’t a knife at all, but a type of extremely precise and sharply focused radiation therapy that treats tumors and lesions in the brain. The precision of the tool is “surgical,” but there’s no cutting, no incisions, and no requirement for anesthesia. Patients are awake and go home after the treatment, resuming normal activities.
The minimally invasive treatment uses a unique technology that produces 200 intersecting beams of gamma radiation. The individual beams pass through the body without causing damage — preserving healthy brain tissue — until the point where they intersect, destroying cancer cells.
Who can receive Gamma Knife treatment?
Patients with brain tumors, brain metastases and select brain disorders. Conditions treated with Gamma Knife at Roswell Park include:
- Metastatic brain tumors and lesions arising from primary tumors of the breast, kidney, colon, skin (melanoma), uterus or other organs
- Brain tumors, malignant or benign, including:
- Meningiomas
- Gliomas (glioblastoma, astrocytoma, oligodendroglioma)
- Craniopharyngiomas
- Hemangioblastomas
- Pituitary adenomas
- Trigeminal neuralgia/tic douloureux
- Arteriovenous malformation
- Acoustic neuroma (vestibular schwannoma)
- Essential tremor and other movement disorders
Advantages of Gamma Knife
New option for recurrent tumors
Recurrent tumors of the skull base and head can now be treated with Gamma Knife, offering a new therapeutic approach to patients.
- Better accuracy. Targets larger tumors with accuracy to within .15 mm, compared to other techniques such as Linac Stereotactic Radiosurgery.
- Real-time dose confirmation. Integrated cone-beam CT imaging and software continuously control radiation dose delivery. If the patient moves out of the target area, treatment automatically stops.
- Frameless fixation. No need for a rigid device attached to the skull, we use other techniques, such as a molded face mask, to hold the patient’s head in position.
- Fractionated treatment delivery. We can treat in multiple sessions, allowing for a higher and more effective overall maximum dose to be delivered more safely and with fewer side effects — even for larger tumors, and tumors close to critical structures.
- Maximizes patient comfort options while maintaining the guaranteed accuracy expected from the Gamma Knife, making it the gold standard for cranial radiosurgery.
Improving outcomes and quality of life
Gamma Knife provides a highly favorable approach to treating the brain compared to next-best methods such as conventional neurosurgery, standard whole-brain radiation therapy and Intensity Modulated Radiation Therapy (IMRT).
At facilities and hospitals without Gamma Knife capability, patients with brain tumors and metastases would likely undergo whole-brain radiation therapy, an approach that exposes all brain tissues to the potentially damaging effects of radiation. With Gamma Knife radiosurgery, only 0.5% of the brain is radiated, preserving significantly more healthy brain tissue and brain function down the road, improving both medical outcomes and quality of life for patients.