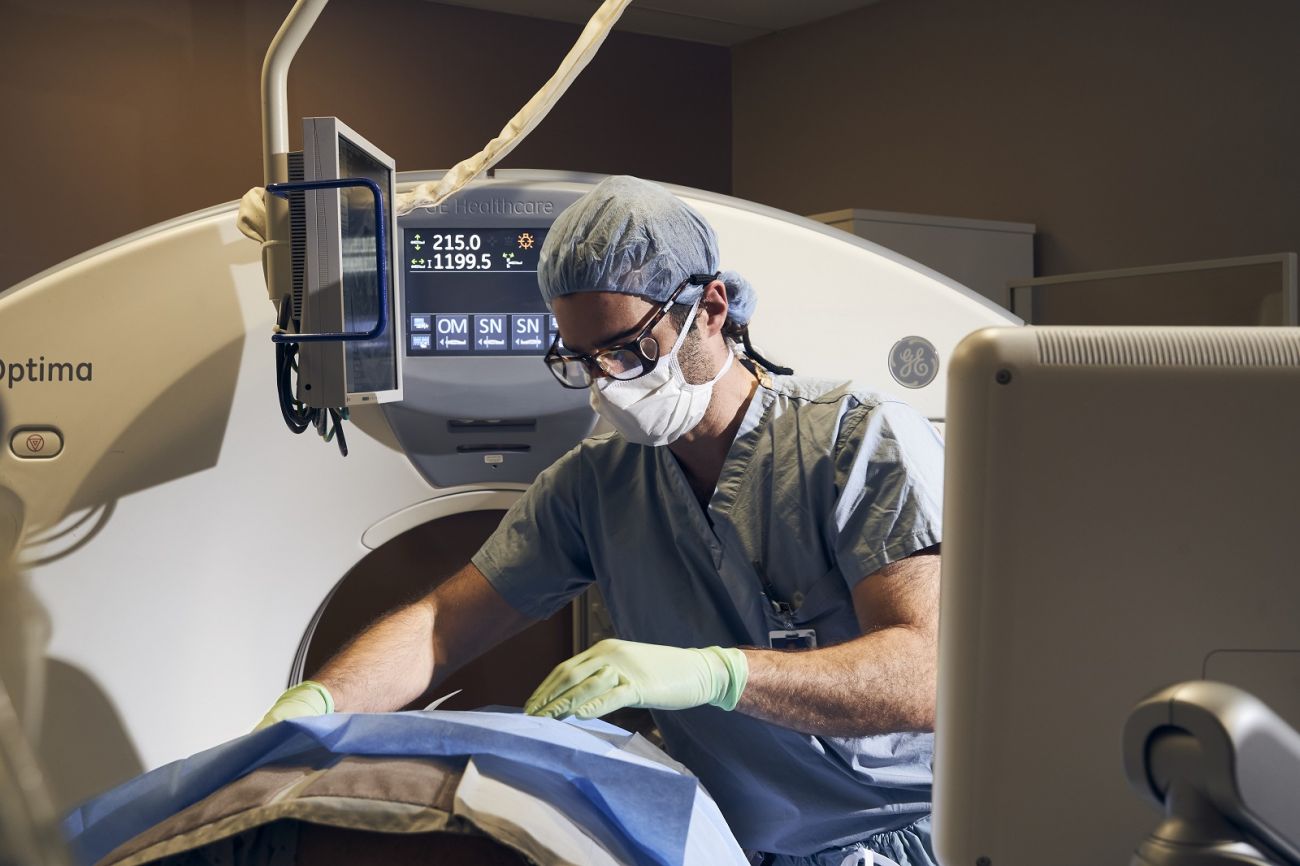
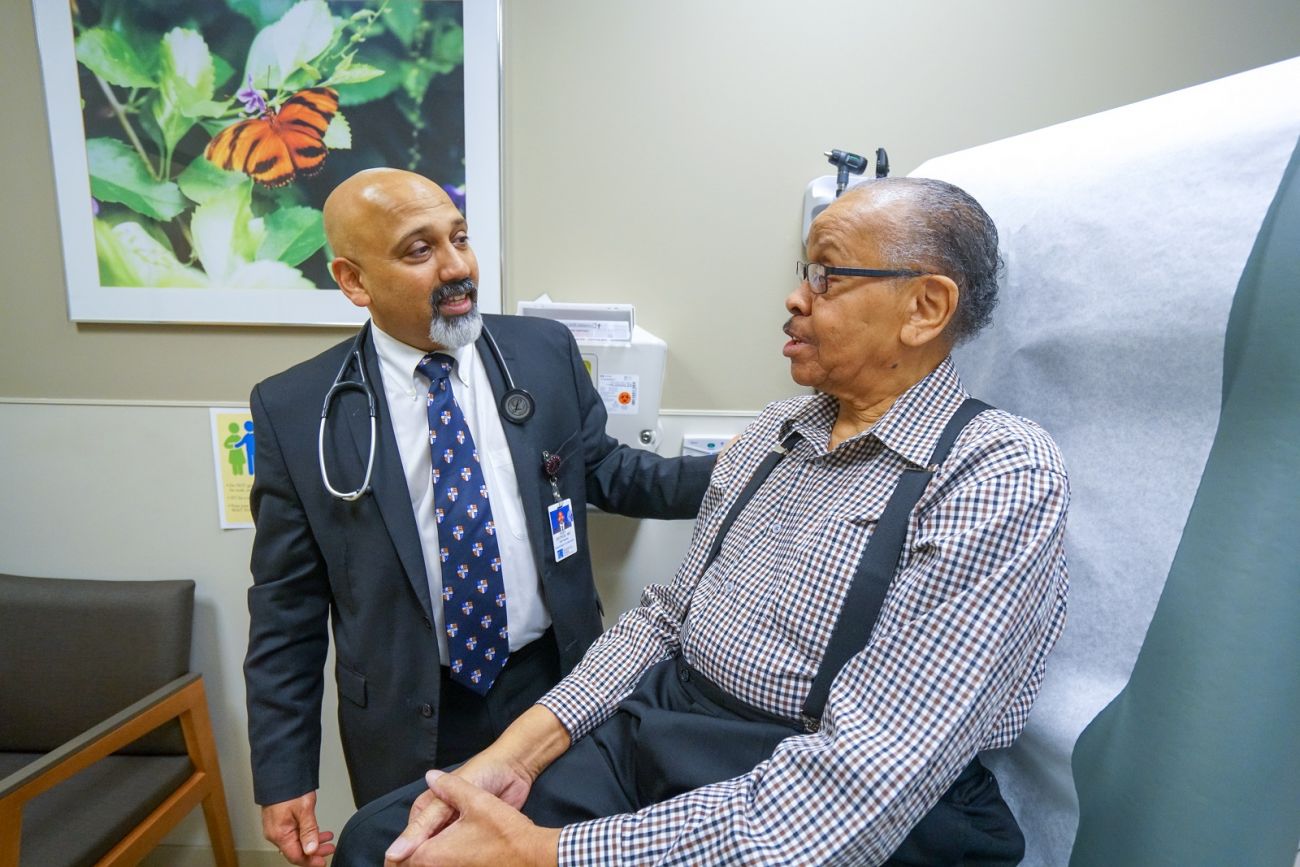
At Roswell Park, you’ll have the expertise of our nationally recognized team of urologic cancer specialists, access to the latest options and the support services you’ll need from diagnosis through survivorship — all in one location.
Why Roswell Park for kidney cancer?
We are designated by the National Cancer Institute as one of the nation’s elite comprehensive cancer centers, and the only one in the state outside of NYC. Learn more about what this means for you.
What sets us apartLatest treatment advances
We offer treatments at the forefront of cancer care and the surgeons and oncologists with the skills and expertise to deliver them safely, looking beyond survival and toward your lifelong wellness for years to come.
Kidney cancer treatmentsActive surveillance — a pioneering approach
Some small kidney tumors do not need immediate treatment and can be safely monitored by our experts and convert to treatment only if your tumor grows — and many don’t!
Learn more